The necessity for a corona virus vaccine causes a progress in the development of new kinds of vaccines. PIRO4D, Pixabay
Currently, doctors can treat the symptoms of Covid-19, but prevention would be better than a cure. That is why scientists from all over the world are trying to develop a vaccine against corona virus. The time pressure leads some researchers to work on new, so called mRNA vaccines. Their development is thought to be achieved much faster and indeed, multiple different kinds are tested already and the first German trial has been approved last week. But what is different about the mRNA vaccine that allows for faster development?
Classic vaccines contain weakened/dead viruses that provoke the same immune response in the body as the living virus, but without causing the illness. In new approaches researchers work with the genetic material of a virus. After injection, a person’s cells start forming parts of the virus envelop. But only those parts that will cause the immune response.
Overall, a minimum of eighty different approaches of corona virus vaccine development are running right now and clinical trials have started for some of them. A new trial was approved for the German company Biontech, in which they will first look for side effects and test wheter the vaccine is save, on two hundred healthy volunteers.
How does a vaccine work?
A vaccine must contain a certain part of the virus which triggers the immune response, this is the so-called antigen. It is found on the virus envelop and is specific for a virus. Specialized cells produce antibodies that can recognize this antigen specifically and tag the virus for its degradation by immune cells. And the organism keeps some of the antibody producing cells as a backup. If the virus were ever to attack the body, the immune system could react much faster and prevent the intruder to propagate, thus, to cause symptoms. As a result, a person becomes immune. This normal response to an infection is called adaptive immunity and a vaccine mimics it, so that we can become immune without ever being sick.
What is different about the new vaccines?
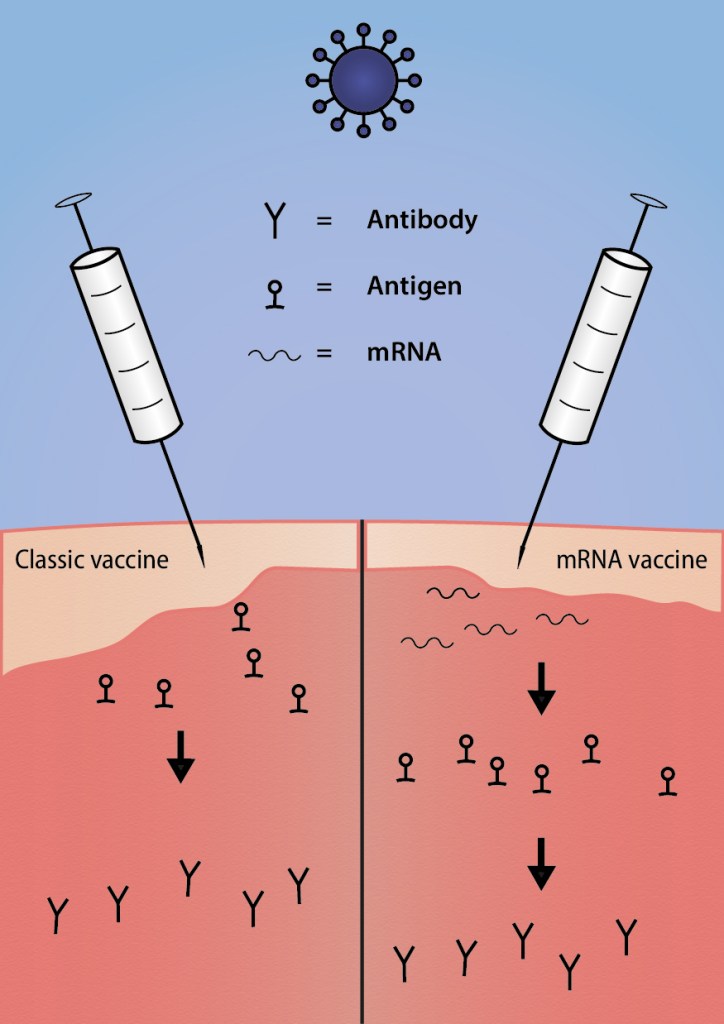
The working principle of the mRNA vaccine is the same as for the classic injections, but scientists hope to reduce the time of development with them. As a main bottleneck of classic vaccine development is that it is time consuming. The researchers must grow the virus and prepare it for injection, by killing or weakening it with chemicals. This demands a lot of effort, not only for the initial development but also for the production of the big batches that will be needed to immunize the world’s population. The new method circumvents working with the virus itself and thus allows for much faster vaccine production.
Scientists first needed to crack the building plan of the virus, its genetic code, to make the mRNA vaccine. It will contain those parts of the building plan that encode the information for the development of the virus’ envelop, and thereby antigen. The cells of the injected person will produce this envelop and this will cause the immune reaction. The idea is copied from the virus itself. It injects its building plan into our cells and forces them to build new, functioning virus that makes us sick.
The difficulty of this method is that the genetic material, the mRNA, is very fragile and needs to enter the cells, which it would not do on its own. It is a challenge for vaccine developers to find a suitable carrier material that can deliver the mRNA into a cell, while keeping it safe. But once it is achieved, production can be much faster than with classical methods. That is why many researchers worldwide are focusing on this approach. The first vaccine of this kind was developed by the US company Moderna Therapeutics, 42 daysafter the genetic code of SARS-CoV-2 was cracked. This is said to be the shortest time period in which a vaccine was ever developed. They are now in phase I of clinical trials, as are others, mainly in the US and China.
How is the effectiveness of a vaccine tested?
The approval of a vaccine is strictly regulated and follows several phases that usually take up to 15 years. We do not have that much time, facing the current pandemic. But there is a debate whether a faster approach is ethical and safe. However, experts agree that there is no other way to tackle the corona virus crisis.
The effectiveness of the substances is normally tested on animals first, this step is now skipped or done in parallel to the safety and tolerability trials on humans. They start with a small number of participants in phase I and gradually increase it up to phase III, to identify even the rarest possible side effects. In addition, they need to determine effectiveness. But will scientists ask a Covid-19 patient to cough at the vaccinated test subject and wait, whether they get the infection too? No, instead they can do laboratory tests to check whether antibodies, specific against the virus, are found in the participant’s blood. Furthermore, they determine the number of antibodies, as a minimum quantity is needed to ensure immunity.
The first corona virus vaccine
The developers of the mRNA vaccines all have slightly different approaches, with regard to which part of the virus’ building plan and carrier material they use. In the end one of them will be the first company to get this kind of vaccine approved, ever. From then on, it will be possible to immunize people on a big scale much faster than it would be with the classic methods.
But experts say that we cannot expect this to happen in 2020. However, this pandemic has surely created the pressure to bring vaccine development to a next level and hopefully we will benefit from this by receiving a corona virus vaccine rather sooner than later.
References
https://horizon-magazine.eu/article/five-things-you-need-know-about-mrna-vaccines.html article from 01.04.2020, written by Joanna Roberts, viewed 24.04.2020, 6:02 p.m.
https://www.sueddeutsche.de/gesundheit/coronavirus-impfstoff-deutschland-biontech-1.4884844 article from 22.04.2020, viewed 24.04.2020, 6:32 p.m.
https://www.statnews.com/2020/03/11/researchers-rush-to-start-moderna-coronavirus-vaccine-trial-without-usual-animal-testing/ article from 20.03.2020, written by Damian Garde, viewed 25.04.2020, 4:59 p.m.
https://www.statnews.com/2020/03/11/researchers-rush-to-start-moderna-coronavirus-vaccine-trial-without-usual-animal-testing/ article from 11.03.2020, written by Eric Boodman, viewed 25.04.2020, 5:27 p.m.
Jackson, N. A., Kester, K. E., Casimiro, D., Gurunathan, S., & DeRosa, F. (2020). The promise of mRNA vaccines: a biotech and industrial perspective. npj Vaccines, 5(1), 1-6.